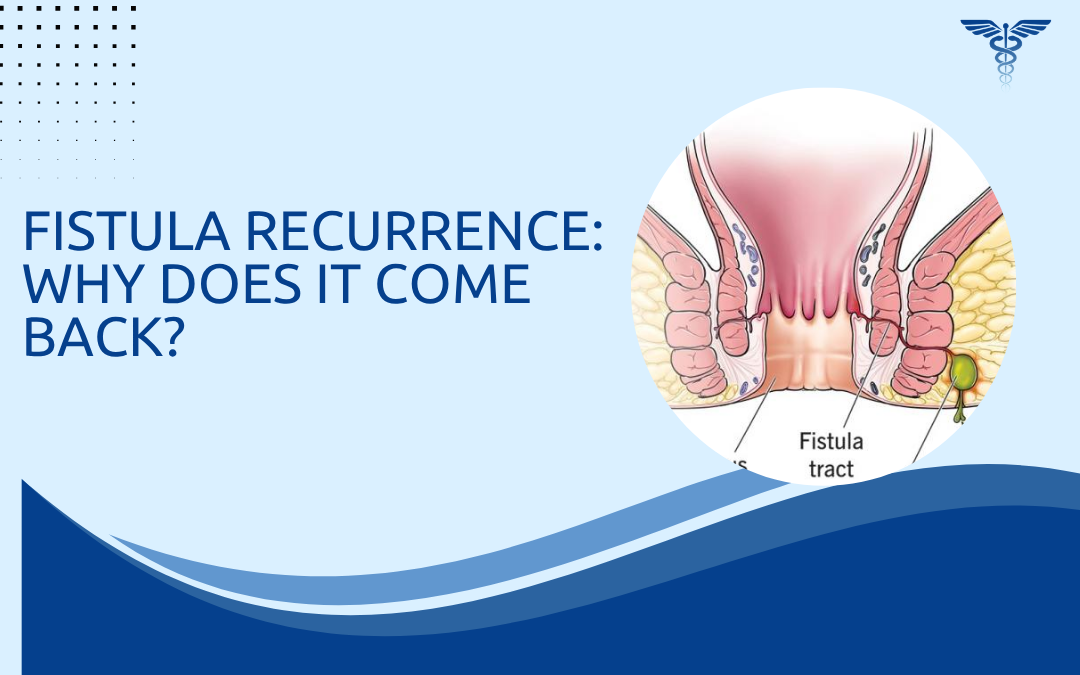
Anal fistula recurrence occurs in 7% to 21% of cases. The most common reasons are incomplete removal of the tract, failure to identify and close the internal opening during surgery and complex branching anatomy that wasn’t fully mapped before the first operation. Underlying conditions like Crohn’s disease, diabetes and tuberculosis cause fistulas to keep returning because the inflammation or weakened immunity driving new sepsis isn’t addressed by surgery alone.
According to Dr. Rajeev Premnath, fistula treatment, “Recurrent fistulas almost always trace back to the first surgery. Either the internal opening was missed, a secondary tract was left behind or the procedure wasn’t matched to the anatomy the MRI showed.”
Recurrent fistula surgery is more challenging and carries higher risk of further recurrence. Getting the first surgery right matters more than anything else in fistula management.
What Are the Exact Reasons Fistulas Come Back After Surgery?
Patients who develop recurrence after fistula surgery consistently describe the same frustration. They thought it was fixed. Then the discharge started again. Knowing which specific factor caused it changes what the second surgery needs to do differently.
- Incomplete tract removal. Not all infected branches were removed at the first operation. A missed side tract or a pocket of infected tissue left behind keeps seeding new sepsis into surrounding tissue. The surface heals. The infection underneath doesn’t.
- Missed internal opening. If the surgeon fails to locate and close the internal opening inside the anal canal the passage reopens. Faecal matter enters the tract with every bowel movement and triggers new infection within weeks of apparent healing.
- Complex anatomy. High trans-sphincteric, horseshoe and multi-branching fistulas are harder to completely fix than simple low-lying ones. Without MRI mapping before surgery a surgeon operating on a complex fistula is navigating blind through anatomy they haven’t seen properly.
- Underlying chronic disease. Crohn’s disease, tuberculosis and HIV all cause fistulas to recur because the underlying inflammation or immune dysfunction keeps creating new perianal sepsis that surgery alone can’t stop. Diabetes impairs healing and high blood sugar at the time of surgery directly increases recurrence risk.
Poor post-operative hygiene also contributes. Skipping sitz baths, missing follow-up appointments and failing to keep the wound clean let the surface close prematurely while infection continues underneath. That’s not a minor issue. It’s a common one.
Patients dealing with a recurrent fistula after prior surgery need full reassessment before any second procedure. The approach to recurrent cases is covered in detail at fistula treatment.
How Is Fistula Recurrence Prevented and Treated?
Prevention starts before the first surgery. Treatment of recurrence starts with admitting why the first one failed and fixing the specific thing that went wrong. Not repeating the same approach and expecting a different result.
- MRI mapping before surgery. Proper pre-operative MRI maps every tract, every branch and the internal opening location before any instrument enters the operating field. Surgeons who skip this step and rely on examination findings alone miss branching tracts consistently.
- Managing underlying disease. Strict control of Crohn’s disease with biologics or immunomodulators, tight blood sugar management in diabetic patients and treatment of tuberculosis or HIV run alongside surgical repair. Surgery without addressing these is treating symptoms not the cause.
- Post-operative hygiene. Regular sitz baths in warm water twice daily keep the wound clean and prevent premature surface closure over an incompletely healed deeper tract. Follow-up appointments at two and six weeks catch early recurrence before it becomes a full abscess.
- High fibre diet throughout recovery. Chronic constipation and straining create sustained perineal pressure on healing tissue. High fibre intake with adequate fluids prevents hard stools and reduces the mechanical trauma to the wound site that contributes to tract reopening.
Recurrence doesn’t mean the fistula is untreatable. It means the specific failure point needs identifying and the second procedure needs to address it directly. That’s fixable with the right assessment.
Read this older piece on top precautions after fistula surgery which covers the post-operative period practically and reduces recurrence risk from the patient’s side.
Why Choose Dr. Rajeev Premnath?
Dr. Rajeev Premnath is a General and Laparoscopic Surgeon with over 20 years treating primary and recurrent fistulas including complex Crohn’s-associated and post-surgical cases. MBBS, MS General Surgery, FRCS Glasgow, trained at IRCAD France. Advanced laser and proctology training completed. Head of Day Care Surgery, Ramakrishna Group of Hospitals.
Patients who had wrong-procedure first surgeries elsewhere come here for reassessment and get a mapped approach that addresses what was actually missed. Repeating the same surgery that failed never makes sense.
Call +91 90082 04466 to book your consultation.
FAQs
How common is fistula recurrence after surgery?
Anal fistula recurrence occurs in 7% to 21% of cases depending on fistula type, complexity and surgical technique used.
What is the most common reason a fistula comes back after surgery?
Incomplete tract removal and a missed internal opening are the two most consistent causes of post-surgical fistula recurrence.
Does Crohn's disease cause fistulas to keep recurring despite surgery?
Yes, ongoing bowel inflammation in Crohn’s keeps creating new perianal sepsis making medical management alongside surgery essential.
Does diabetes affect fistula healing and recurrence risk?
Yes, high blood sugar significantly impairs wound healing and increases the risk of infection and tract reopening after fistula surgery.